A multi-institutional team including Yale School of Medicine (YSM) Yale School of Medicine (YSM) led by Dr. Raimund Herzog has demonstrated the use of ultrasound which stimulates specific neurometabolic pathways in the body. Because of this, the body will make insulin and diabetes can be cured. The team published this study in Nature Biomedical Engineering.
Insulin
Type 2 diabetes is an impairment in the body in how it regulates and uses sugar (glucose) as a fuel. This long-term condition causes too much sugar to circulate in the bloodstream. Eventually, because of such heightened blood sugar levels, one gets predisposed to disorders of the circulatory, nervous, and immune systems.
In type 2 diabetes, your pancreas does not produce enough insulin, and cells respond poorly to insulin and take in less sugar. This chronic condition affects millions of people all over the world. It is a major cause of blindness, kidney failure, heart attacks, stroke, and lower limb amputation. Several studies are being regularly conducted to find the most effective treatments.
New ways
“Even though we already have a large variety of anti-diabetic medications available to us to treat high glucose levels, we are always looking for new ways to improve insulin sensitivity in diabetes,” Herzog said in the press release of the Yale University. “Unfortunately, there are currently only very few drugs that lower insulin levels.”
“If our ongoing clinical trials confirm the promise of the preclinical studies reported in this paper, and ultrasound can be used to lower both insulin and glucose levels, ultrasound neuromodulation would represent an exciting and entirely new addition to the current treatment options for our patients.”
Raimund Herzog’s team discovered novel insights into the molecular mechanisms underlying brain energy substrate metabolism. Thereby laying the basis for the development of targeted therapies that will protect the brain from diabetes complications and injury.
They used ultrasound treatment on blood glucose. He quoted that although there are a large variety of anti-diabetic medications available to treat high glucose levels, it is still important to find new ways to improve insulin sensitivity in diabetes.
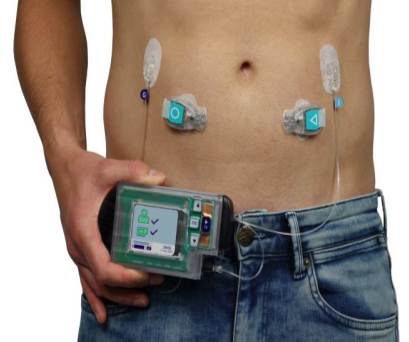
Signals to the brain
In the study, the ultrasound pulses were used to activate metabolic sensory nerve pathways in the liver-related to glucose management. Typically, the sensory nerves of the liver can increase or decrease signaling to the brain during different metabolic events (such as feeding or fasting).
The ultrasound pulses instigated the sensory nerve signaling towards the metabolic control centers in the brain. Ultimately, the effect of the ultrasound pulses was demonstrated to prevent or reverse the onset of high glucose in multiple species and models of type II diabetes.
Currently, Raimund’s team has started with the next step in their study where they are conducting human feasibility trials with type 2 diabetic subjects. This move seems promising for a future where diabetes treatment will no longer require blood sugar tests, insulin injections, or even pharmacological drugs. The goal of such studies is to come up with an effective and long-lasting treatment for type 2 diabetes.
Breakthrough
The reported findings are an important addition to the applications of bioelectronic medicine. Currently, bioelectronics is being used to treat chronic diseases such as diabetes using novel medical devices to modulate the body’s nervous system. At present, the collaborators are also conducting additional studies that investigate the effects of alternate dosing such as the type of ultrasound pulse and duration of treatment. The results of which can be expected later this year.








