February 4 is World Cancer Day that takes place annually to unite people, communities and institutions in the global fight against cancer, to raise awareness and to educate about cancer. Researchers are continuously looking for ways to establish new viable cancer treatments. Here are the stories about three innovative approaches to anti-cancer therapy that are likely to change the ways cancer is treated in the future.
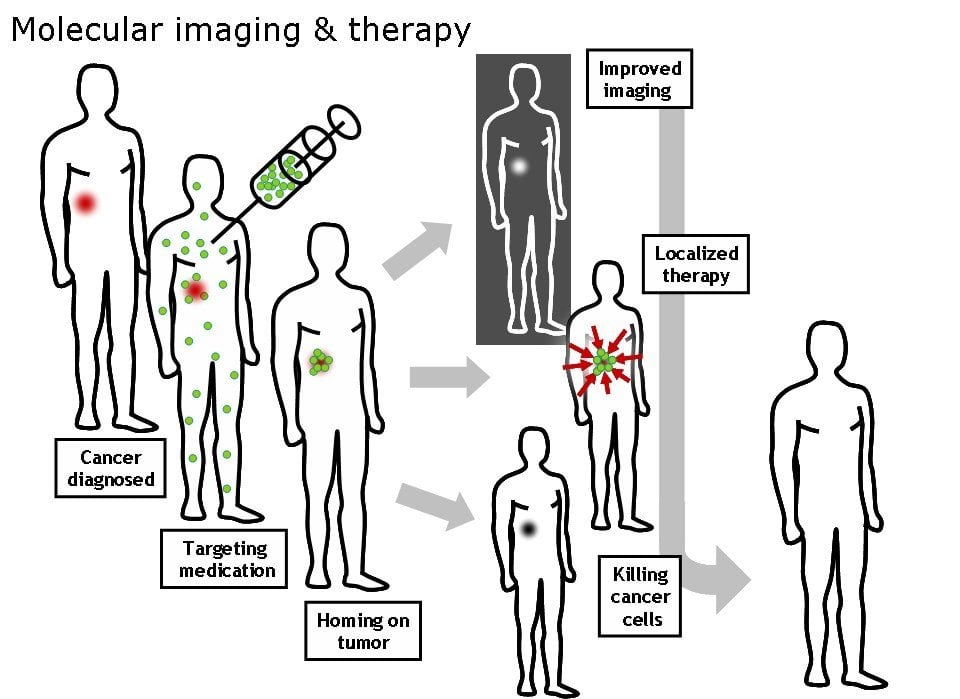
Molecular imaging is a scientific and technological field which aims to obtain information on biological processes at the molecular and cellular levels in a human body in a non-invasive way; it identifies and characterises processes that are going on in the body. Molecular imaging is used for the cancer diagnostics and treatment: for example, in a form of PET (Positron emission tomography), which visualizes the metabolism in the cells by administering a variant of glucose that is labelled with a radioisotope. PET imaging technology can indicate the sites of the body where the increased metabolic activity is localized. Cancer cells have a high metabolism, so molecular imaging visualizes these cells in the body. When the anti-cancer therapy is given to a patient, it is possible to follow the efficacy of the treatment with the molecular imaging technique observing if the cancer cells are disappearing.
“The challenge for the molecular imaging nowadays comes from the clinicians working with the cancer patients,” tells us Chris Reutelingsperger, the chief scientific officer of the company PharmaTarget that works on innovative molecular imaging components. “Clinicians need to know as quickly as possible if the anti-cancer therapy that they are giving to the patient is working. Currently, a clinician has to wait for 4-6 weeks after the start of the treatment before diagnostic procedures such as PET scan are able to report the efficacy of the therapy. This implies that a patient can be exposed to a toxic treatment for weeks without any beneficial effects of the treatment.”
“If the therapy is effective, this will happen within 24-48 hours. If it determines that the current therapy doesn’t work, the clinician can quickly change it to another.”
According to Reutelingsperger, one of the goals of molecular imaging is to offer the clinicians the means to determine the efficacy of a treatment as quickly as possible after the start of the treatment. “Anti-cancer therapies aim at killing the cancer cells. In most cases, the killing process involves the activation of apoptosis – a regulated process of cell suicide. Apoptosis has a specific molecular signature, so one can distinguish cells in apoptosis from the living cells – on the basis of specific molecules. One of those signatures of apoptosis is a specific phospholipid, the so-called phosphatidylserine, which can be detected with the protein called Annexin A5,” says Reutelingsperger. “What we did was the following: Annexin A5 was labelled with a radioactive isotope that is used in nuclear medicine in the clinic. Radioactive Annexin A5 was injected into the bloodstream of patients. Depending on the nature of the radioactive probe, you can use either SPECT (Single-photon emission computerized tomography) technology or PET technology to localize the protein in the body and, thus, to localize and to estimate the number of cancer cells in apoptosis. The nuclear medicine physician can measure a certain amount of uptake of Annexin A5 in the tumour before and 24-48 hours after the start of the treatment. An increase of the uptake of Annexin A5 induced by the therapy indicates that therapy has caused an increase of apoptosis in the tumour, and, hence, shows that the therapy is being effective. Oppositely, if there is no increase of uptake, it shows that the therapy probably is ineffective. In that case, the clinician can decide relatively quickly after the start of treatment to change therapy.”
The Annexin A5 platform is developed by PharmaTarget in Maastricht Health Campus. “We are developing molecular imaging protocols and targeted-drug delivery systems based on Annexin A5. Currently we are developing those for pre-clinical studies, and we are preparing the base for clinical trials with patients,” says Chris Reutelingsperger. “Therefore, we are delighted with the recent initiatives at Brightlands Chemelot Campus where Basic Pharma develops a Good Manufacturing Practice (GMP)-facility to produce small scale GMP-batches of biologicals for the first phases of clinical studies. Such a facility is crucial for small biotech companies that develop diagnostic and therapeutic products of biological nature such as, for example, Annexin A5.”







