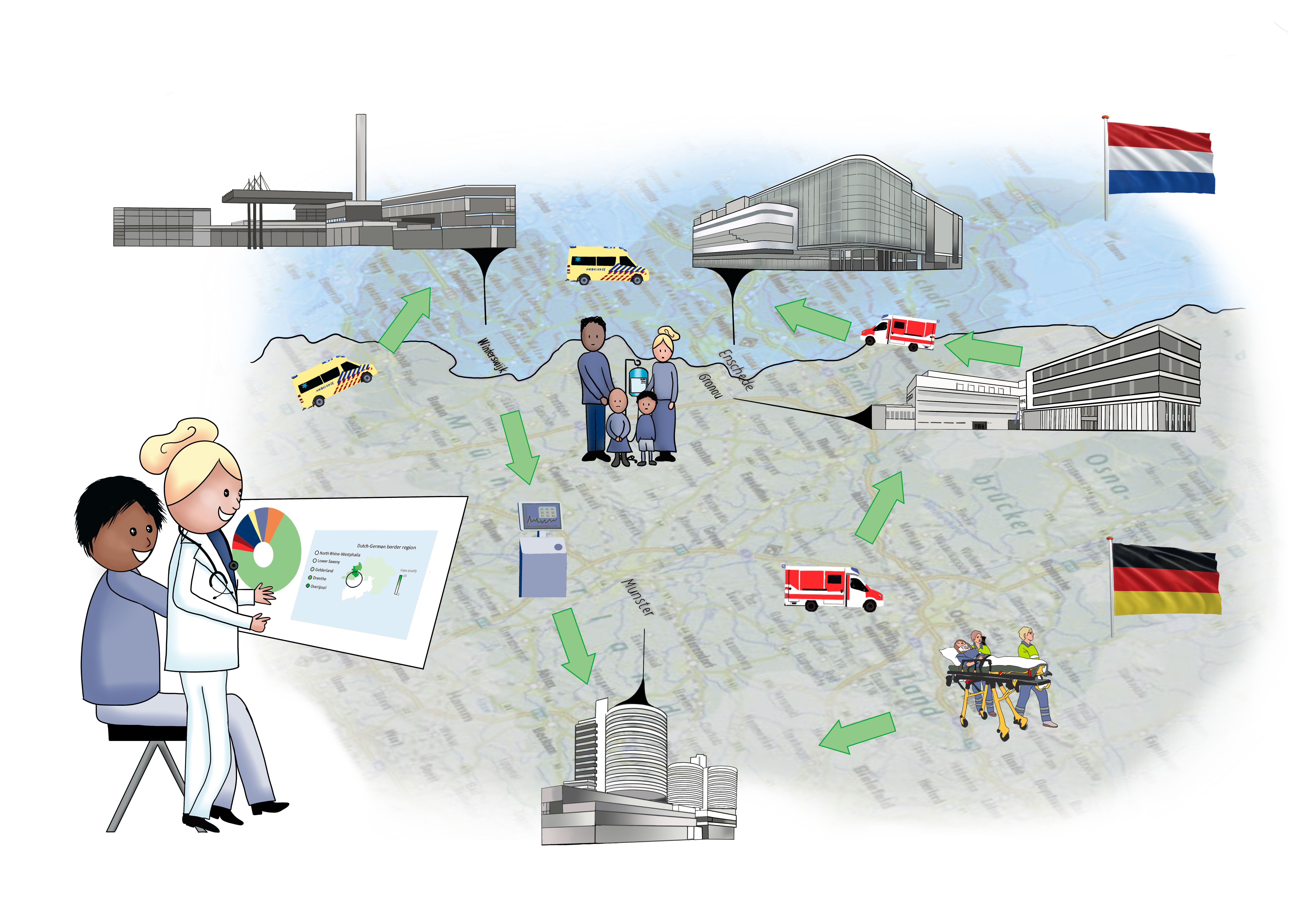
The RAPIDE consortium (Regular and Unplanned Care Adaptive Dashboard for Cross-border Emergencies) is led by Radboudumc Professor of Primary Care Aura Timen and receives €5.9 million from the European Commission. Radboudumc announces this today in a press release.
- A European consortium of seven countries, led by Aura Timen of Radboudumc, receives 6 million from the European Commission.
- The project focuses on developing and testing scenarios and care models to organize regular care more flexibly and resiliently during health crises;
- Rethinking patient flows, access to regular care, and providing up-to-date and understandable information to the public are key topics.
“During the COVID-19 pandemic, a great deal of regular healthcare across Europe was adjusted, postponed, or even stopped,” says Timen. “The entire spectrum of care was disrupted, from elective surgeries to chronic conditions, cancer care, and mental health. Many people also chose to avoid necessary regular care and, for example, did not visit their general practitioner or hospital, despite having health problems.”
Patient flows
Disrupting or interrupting regular care during a pandemic or other health emergency can have long-term consequences for patients and healthcare systems. Learning from our experiences during COVID-19, and building on research into healthcare optimisation and forecasting, the new project will create and experiment with more flexible and adaptable ways to deliver healthcare. Greater use of community and at-home care can help to make acute hospital resources available to deal with crises; they can also help to improve healthcare efficiency during ‘peace-time’.
Part of this research involves restructuring patient flows during health crises. Timen explains, “We are exploring whether we can relocate care. Can patients stay at home more often? And if so, what is needed for this? This relocation could involve tools closer to the patient, such as more online appointments or apps that provide training programs and directly report progress to the hospital or attending (primary care) physician.”

Living labs
The research results, in the form of practical, flexible models of care delivery during health crises, will be tested in real-world settings known as living labs. Scenarios and care models will be explored and assessed in collaboration with healthcare providers and patients, across hospitals and primary care, in four different European countries. Additionally, the study will explore how we can adapt such flexible care models to the healthcare systems of other European countries.
In the Netherlands, the partners include Radboud University, RIVM (National Institute for Public Health and the Environment), the University of Twente, and HAN University of Applied Sciences. International partners include institutions, companies, and organizations from Slovenia, Norway, Ireland, Italy, Malta, and Estonia, as well as the European Forum for Primary Care.