Multi-resistant germs evoke the specter of terror for people who have to go to the hospital. According to information from the German Federal Ministry of Health, 400,000 to 600,000 people in Germany contract infections every year that they have caught during in-patient treatment. As a result, between 10,000 and 15,000 people die in Germany and more than 30,000 throughout Europe.
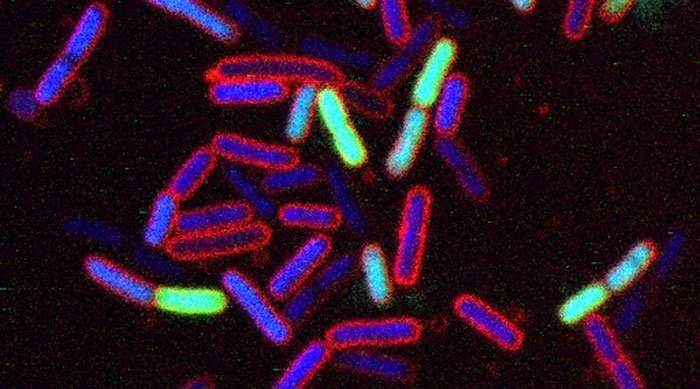
The problem is that many bacterial pathogens are now immune to several classes of antibiotics. According to the World Health Organization (WHO), “Gram-negative bacteria with resistance to carbapenem and cephalosporin antibiotics” pose a growing threat because they can cause serious infections such as pneumonia or meningitis, wound infections or blood poisoning. The reserve antibiotic colistin is often no longer effective against these often life-threatening infections.
New mechanism of action
In the fight against these pathogens, researchers led by Anatol Luther of the pharmaceutical company Polyphor AG in Allschwil and Matthias Urfer of the University of Zurich have now developed a new class of antibiotics that can apparently also neutralize dangerous Gram-negative pathogens such as Escherichia coli, Klebsiella or Pseudomonas. The antibiotics interact with proteins of the outer membrane of Gram-negative bacteria,” said Urfer’s colleague John Robinson. “According to our results, they bind to fat-like membrane components, the so-called lipopolysaccharides, on the one hand, and to the BamA membrane protein on the other.
More articles on multi-resistant germs can be found here.

By binding the antibiotics to BamA, the main component of the so-called beta-folding complex (BAM), which is essential for the synthesis of the bacterial outer membrane, the membrane, an important protective envelope of the pathogens, is destroyed. The outer membrane not only protects the bacteria from toxic environmental factors and antibiotic attacks, it is also responsible for the uptake and export of nutrients and signaling molecules.
Robinson explains that none of the clinically used antibiotics would target key proteins that are required for the biogenesis of the outer membrane. However, investigations using cell cultures and mice infected with bacteria have shown that this strategy is effective. The destruction of the outer membrane leads to the bursting of the cells and thus to the containment of the infection.
New miracle weapon against hospital germs?
After some of the substances tested even showed significant activity against various multi-resistant pathogens such as the ESKAPE pathogens, a group of dangerous hospital germs, they will be tested in human studies as soon as possible.
According to co-author Daniel Obrecht of Polyphor, an initial lead molecule of the novel antibiotic class is currently in preclinical development. If the active substances prove to be effective, they could be the first antibiotics on the market since the 1960s that combat these Gram-negative bacteria. “This would have the potential to effectively combat life-threatening infections and thus meet an urgent medical need,” explain the researchers in their study, published in the journal Nature.