In medical research, experiments are still being carried out on millions of mice, rabbits, rats, dogs and monkeys worldwide, even though it has recently become increasingly difficult to obtain approval for animal experiments. In biomedical basic research in particular, researchers repeatedly stress the great importance of these animal experiments. Diseases such as cancer, dementia, heart disease or diabetes are still considered incurable. Animal experiments are therefore indispensable for testing new drugs, for example. But is that really true?
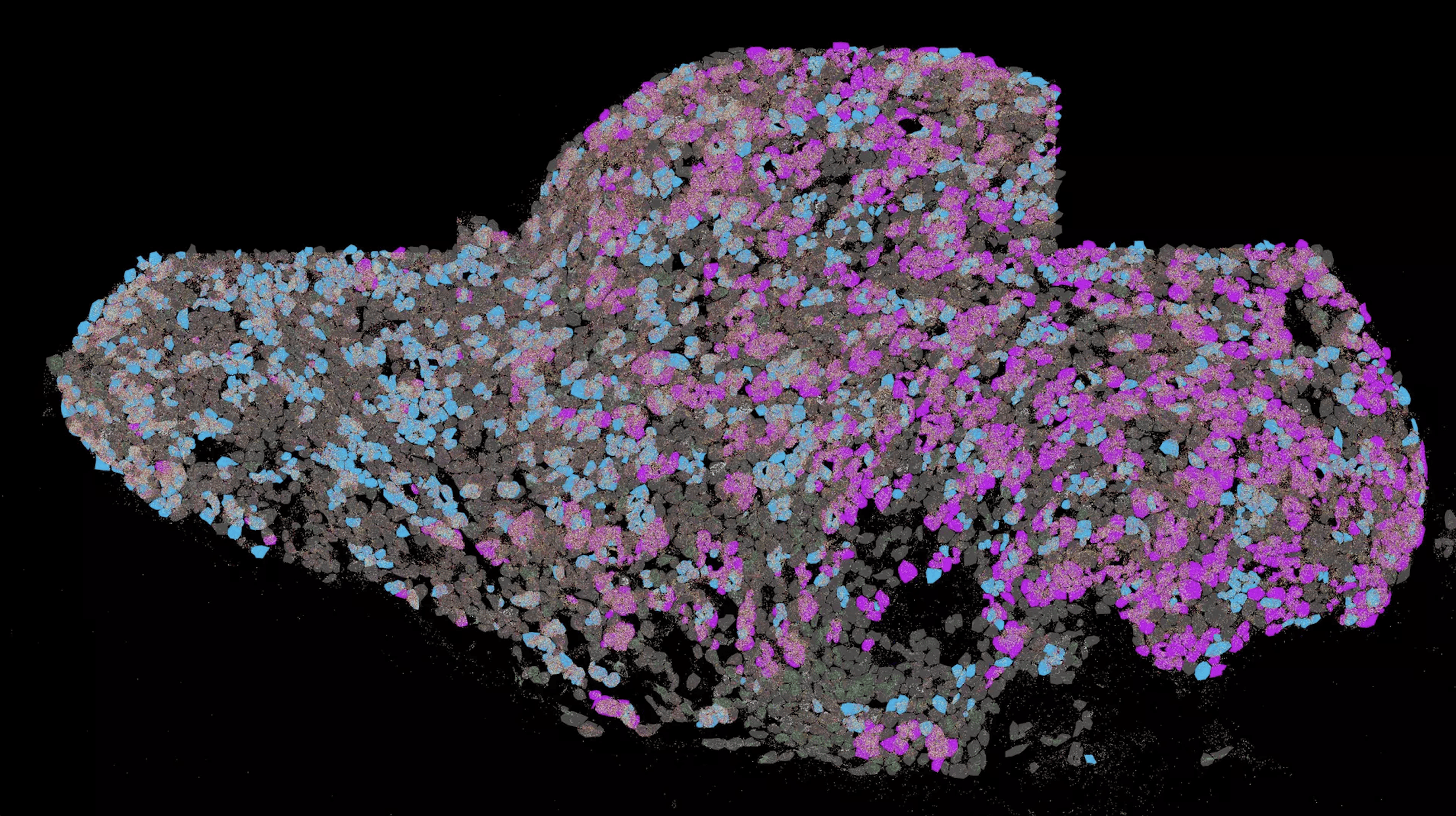
No, says Dr. Joachim Wiest, Managing Director of the Munich-based company cellasys. “Here we have the opportunity to simply take cancer cells, which can be ordered from the German Collection for Microorganisms, monitor them with this system and add new medicines. The lab-on-a-chip technology developed by cellasys enables scientists to obtain meaningful results on the basis of tests on individual cells in the same way as with conventional animal experiments.
“In cancer research, personalised medicine involves taking a biopsy from a cancer patient, applying it to the system and knowing which drug will work best before therapy begins”, explains Wiest. By testing different drugs and exclusion procedures, it would be possible to select the best drug for the respective patient before starting therapy. “This is particularly true for patients who have already undergone therapy and who have already had a lot of trials. With such a technology one could see what still works and what no longer works.”
Read the whole series about cellasys HERE
A dream of the future
However, the emphasis here is on ‘could’, because unfortunately, such individualized chemotherapy is still a dream of the future and patients must wait further until this method will be in clinical use. “It is scientifically proven that this possibility exists, but the official approval is very lengthy and very expensive. It takes years to decades,” says Wiest. “We had a project with the Cancer Research Center in Heidelberg. They looked at the technology and were convinced of it and we were supposed to examine 1,000 patients with it. However, the examination of a patient costs 2,000 euros, with 1,000 patients this is 2 million euros which cellasys would have had to raise.” For a small company like cellasys this is, of course, impossible and so this investigation could not take place. Moreover, this investigation would not have led to an approval of the procedure for a long time.

© P.Wiesmayer
“We’d only be at the next step. Basically, cellasys has started to provide individualized chemotherapy. But then we saw that market access is so difficult and that you can’t run a small business with it. Therefore, we did not focus on personalized chemotherapy, but on toxicological investigations with a lab on a chip.”
At the moment there are no industrial users, the system only runs at universities. “A system that is also used for research is located in the Klinikum Rechts der Isar in Munich and we also cooperate with the Technical University of Munich,” says Wiest, who also lectures at the TUM.
Hope for diabetics
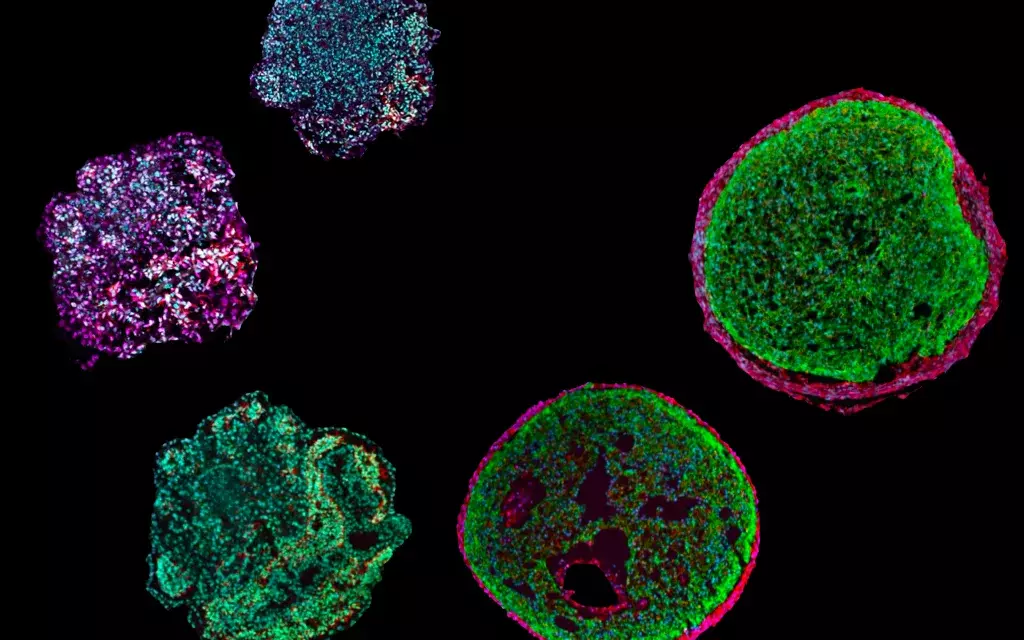
A joint project with the TU Munich already existed in the field of regenerative medicine. “It was about curing diabetes by transplanting pancreatic cells. Diabetics do not produce insulin, the pancreas is responsible for this, which is why the idea was to take healthy pancreas cells and transplant them,” said Wiest. “Pancreatic islands, in particular insulin-producing beta cells, can be monitored under various nutrient supply conditions. The metabolic measurement of beta cells or islets can provide basic information about their viability and functionality in regenerative medicine.”
However, the difficulty is that it is only possible to transplant once because the transplantation triggers the immune system. “The second time, the cells are immediately rejected. This means that you should use as many vital beta cells as possible for this first shot. We have shown that our technology is well suited to select the most vital cells.”
However, the method is suitable for a wide range of applications, such as heart failure, the cartilage replacement or “when an organ has a problem”, as living cells can be examined and the quality of biological material assessed, which is then used in regenerative medicine. These living three-dimensional cell constructs required for such experiments can be produced in the laboratory on a patient-specific basis, be it heart cells, skin cells, liver cells or the like.

© cellasys
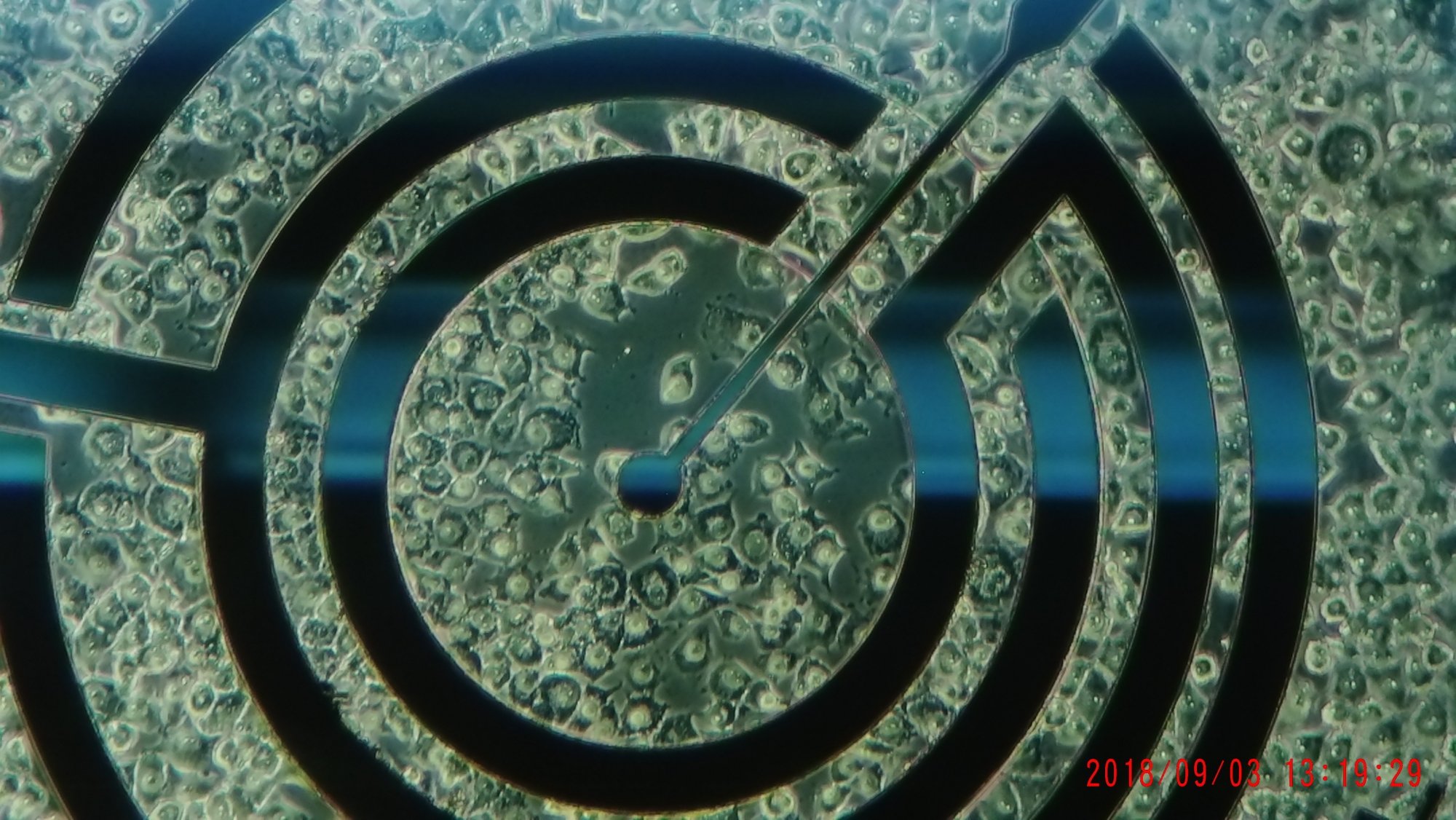
“The biochip contains miniaturized pH sensors, oxygen sensors, temperature sensors and impedance sensors,” explains Wiest. “If cells grow on this chip, the pH value and oxygen can be measured, how strongly the cells adhere to a surface and one can see how strongly the cells change the pH value in their environment. With a special system, these values are read out and medicines, active substances, chemicals, whatever are added. You can see directly how the cells react to it.” This procedure runs fully automatically over hours, days and weeks. “No lab worker has to pipette anything, it’s all automatic. We’ve developed fluidic systems that run autonomously for a month.”
The whole thing is monitored, carried out and recorded in the IMOLA laboratory, where the sensors are electronically read out. “Here you can see, for example, how much oxygen the cells consume. They are simultaneously connected to a fluidic system that provides them with the optimal nutrients to survive on the system.”
Of course, the aim of the experiments is not only to keep cells alive but also to see how they react to certain irritants such as chemicals when testing new cosmetics. “You can switch back and forth between media and add, for example, a certain concentration of a chemical or nutrient that we want to study. All this takes place in a heating cabinet heated to 37° in order to be able to simulate the situation on the human body as faithfully as possible.”
Market leader
The parameters are read out automatically every 5 seconds, which means that after one month there is a huge amount of data that needs to be evaluated. Only then do people come into play again, which makes cellasys the market leader for such systems. “To my knowledge, there is no comparable system,” says Wiest. “There are some who can also study and read cell models for a month, but this always has to happen with a human, there is no other automated model.
Besides the possibility to run autonomously for one month, IMOLA has another special feature that distinguishes the system from others. “We have modified the fluidics in such a way that we can pump a medium onto the skin model on the chip, but it can also be removed again. This is even closer to the real conditions on human skin. Normally you have cell cultures in the Petri dish, but we also have an automated Air Liquid Interface.”
What lab on a chip and IMOLA can do in the field of basic research and environmental monitoring can be read in the third and last part of our small series.