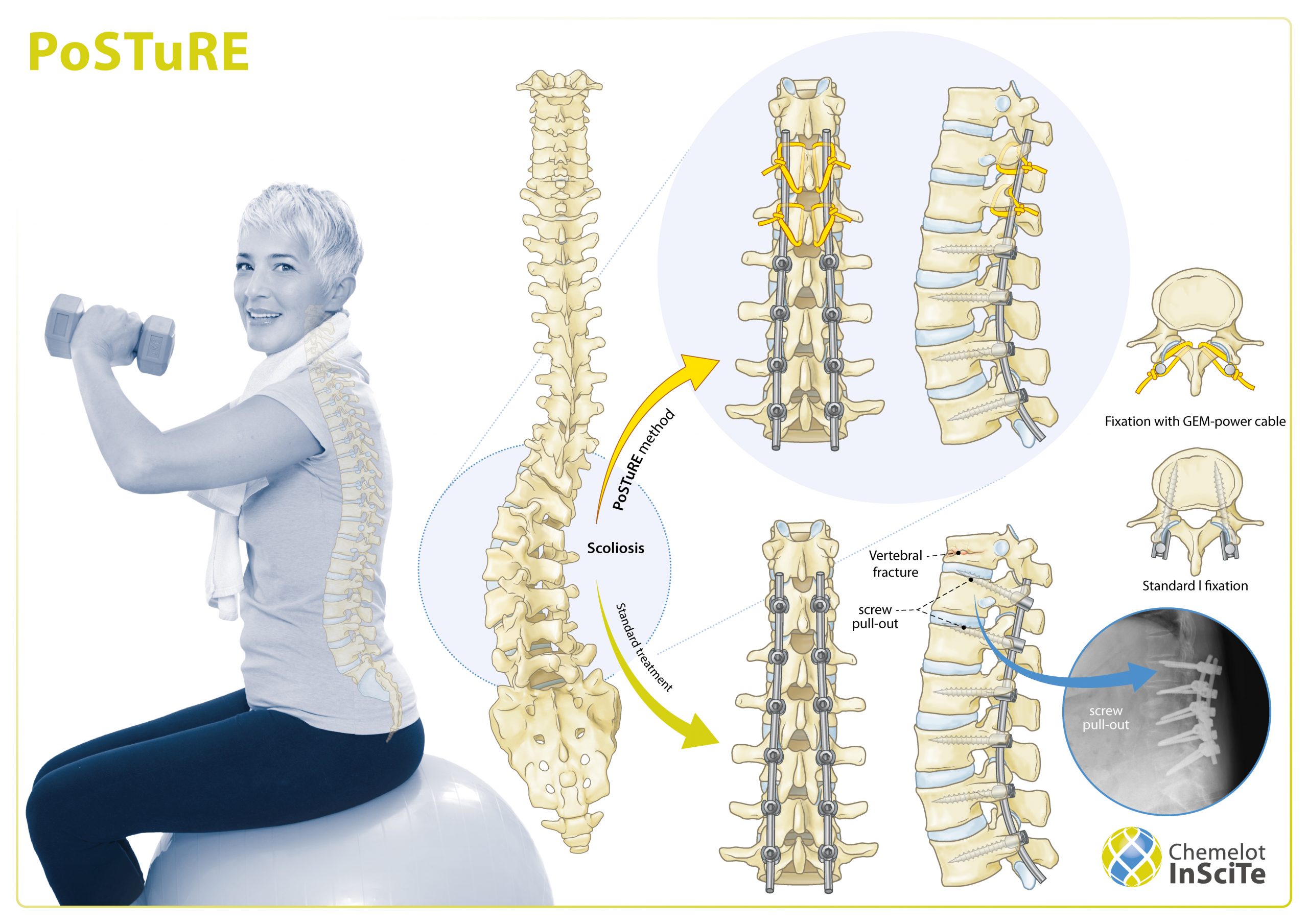
In the Netherlands, 4 out of 1,000 people suffer from scoliosis. Every year about 600 patients are operated on. Scoliosis is a condition in which the spine grows crooked, creating curvatures in the back that can cause a bulge. The condition can be congenital but can also be caused by wear and tear of the joints or incorrect posture. In serious cases surgery is necessary.
During the operation, the spine is straightened and secured with metal screws and rods. The purpose of this is to restore the curvature and stabilize the back. In young patients (<10 years) this operation sometimes has to be repeated several times to ensure that the back can continue to grow.
In older patients, the back is no longer growing, but the spinal column might not fit together properly, a vertebral fracture could occur at the transition areas or a screw could break, making it necessary to operate again. In addition to these complications, osteoporosis or porous bone can also cause difficulties in these patients.
PoSTuRE
PoSTuRE or Patient Specific Scoliosis Treatment, a project of Chemelot InSciTe, is introducing a new treatment. It foresees that the metal screws used in the surgery be partially replaced by woven polyethylene, plastic and cables. The problem of broken screws is eliminated by cables that secure the bone of the vertebral arches instead of screwing. Researchers of the project are confident that this treatment will drastically reduce the number of repeat operations.
Chemelot InSciTe is collaborating on this project with Eindhoven University of Technology, Maastricht UMC+, the Dutch multinational corporation DSM and Xilloc Medical BV.
The method
Filip Maes, senior project manager Biomedical Projects at Chemelot InSciTe says: “In scoliosis, the side, front and back of the spine grow crooked. This can cause growth problems in children. As a result, some organs cannot develop properly, which can lead to complications such as lung problems. The procedure that currently exists for this is quite intense. Screws about the size of an index finger are drilled into the spine. Patients are left with large scars and complications still occur too often.”
“We have researched a new method using a specially woven cable of strong ethylene-based fibers which should enable us to operate better and more effectively. We use a conductor to wrap the wire around the vertebral arch, then fix it with a so-called tensioner at the right tension. The tensioner is an extra device that ensures the right balance. So this project actually consists of three different innovative products: the cable, the conductor and the tensioner.”
Clinical studies
“Last week we received permission to start clinical trials on adult patients at the beginning of next year. For the time being, this approval only applies to adult patients. We will first determine whether the method of adult surgery is safe and works before looking at treatment for children with scoliosis,” says Maes.
Paul Willems is an orthopedic surgeon at Maastricht UMC+ and the project leader of PoSTuRE. “For elderly people with scoliosis, we want to fix the spine in the right shape. In younger patients, we want to fix the spine such that these patients can continue to grow. The cable we developed is suitable for both of these situations.”
Quality
“Maastricht UMC+ is the sponsor of the clinical research. This is a big step for the hospital because this is the first time that it has the role of being in charge of clinical studies. They are actually responsible for bringing the three products together. The hospital has to comply with comprehensive regulations that guarantee product quality and patient safety.”
“Several quality control employees are responsible for assessing whether the study meets all the requirements. Clinical Trial Center Maastricht helps and advises us in setting up our research. In the trial phase, we want to operate on twelve adult patients. Subsequently we must keep a close eye on them, especially during the first six months, because this is when most complications occur. In total, the study will take five years.”
“Eindhoven University of Technology created a digital model with which the forces that work in the back can be predicted and optimally distributed. Thus the program can specifically predict where a cable and a screw should best be placed. In this way we reduce the risk of possible complications.”
Partners
Maes adds: “We launched the project in December 2016 as the pilot project of InSciTe. We went from product to clinical trials at high speed both in terms of setting up and carrying out the trials. Our task was actually to create a network by bringing in expertise that was lacking in the team to make sure that the product would actually come together.”
“There are many partners involved. For example, the cable is being developed by Dutch multinational corporation DSM in the Netherlands and the conductor by DSM America. InSciTe now works with more than 35 partners and knows exactly who has what expertise in-house. By bringing them together, we are accelerating the development process to make innovative medical products available to patients sooner.”
Future
Willems comments: “Standard adult surgery causes complications in about one in three patients, requiring repeat operations. With the products we develop, we hope to drastically reduce these figures.”
“If the first trials go well, that will show that the product is safe and its effectiveness can be measured. This process will take several years, so it will be some time before we can begin performing surgery on children, probably three to five years. In the next two years I hope to operate on twelve patients for the clinical trials.”
Chemelot InSciTe not only works on projects related to orthopedics, but also on biomedical projects in the field of ophthalmology and the cardiovascular system. An overview of all biomedical projects can be found on the website.