Research into the cholera bacterium has yielded a new therapeutic approach that can be applied to almost all infectious diseases. New drugs developed on this basis can replace antibiotics. As a result, the natural microbiome in the intestine is spared.
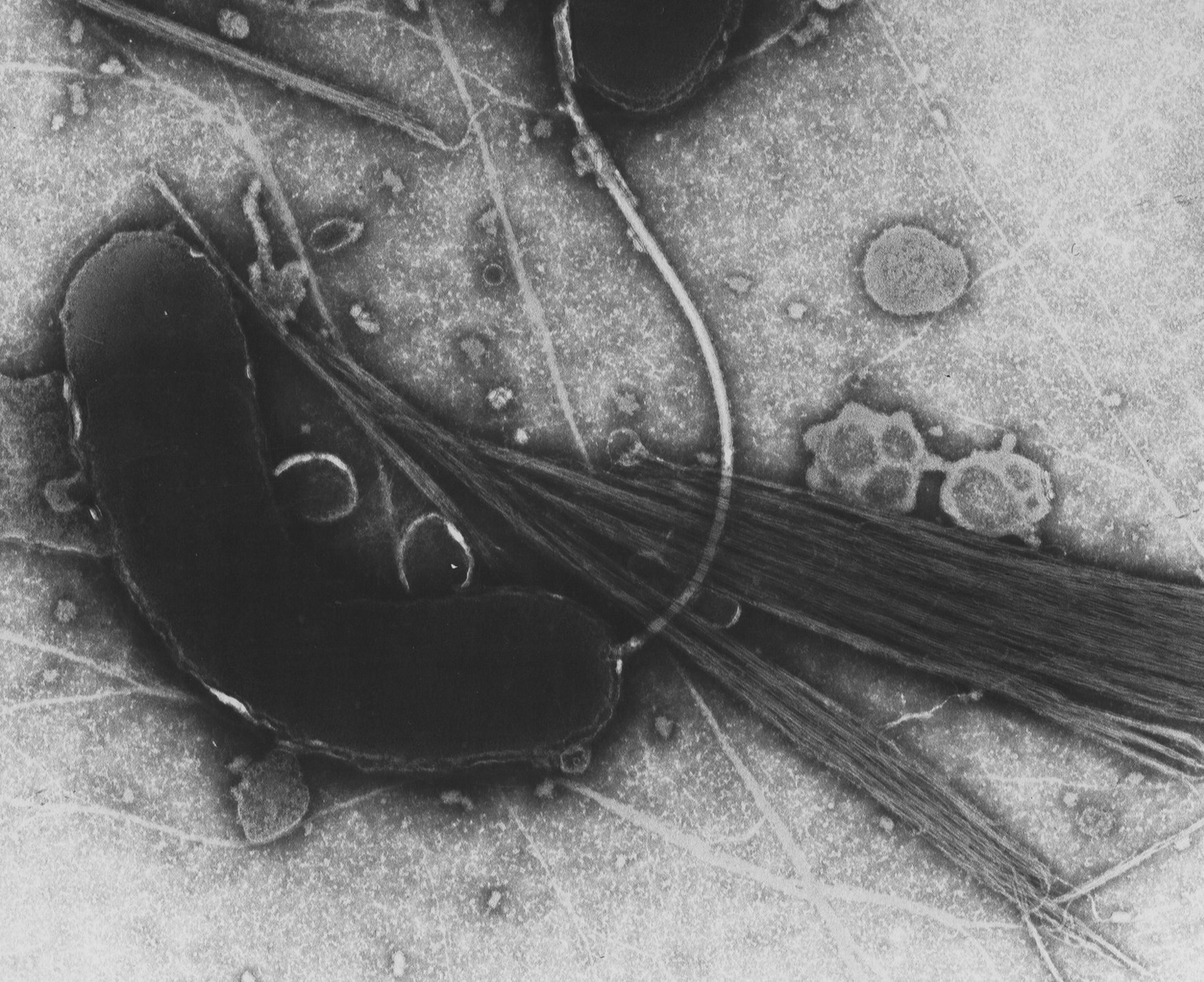
Cholera is a serious bacterial infectious disease caused by the bacterium Vibrio cholerae. The infection usually occurs via contaminated drinking water or contaminated food. If cholera is not treated, the mortality rate can range from 20 to 70 percent.
Between epidemics, the cholera bacterium survives in water where it has to contend with very different conditions than in the human body. Until now, it was not known how the mechanism responsible for the survival of the cholera bacterium works in this totally different environment.
Cholera bacteria can adapt
PhD candidate Franz Zingl of the Institute of Molecular Biosciences at the University of Graz, Austria, has now discovered that the outer membrane vesicles (OMVs) of the cholera bacteria are responsible for this extraordinary adaptability. OMVs are protrusions of the outer skin that can repel the cholera bacteria by cordoning off. This process is very energy intensive. It helps the microorganisms to adapt more quickly to adverse host conditions – and to escape the immune system.
Changing the diet
The outer skin of cholera bacteria is also responsible for its nourishment and has numerous nutrient absorption systems, including the so-called Porin OmpT. In the human body, the bacteria would thus absorb bile salts and anti-microbial peptides which would be fatal for the bacteria. To prevent this, the bacteria stop producing new Porin OmpT. Until now, it was unknown how that works.
Strengthening resistance
Zingl and his team succeeded in demonstrating that the pathogens massively repel the bulges of the outer skin when entering the host. This is the mechanism by which the cholera bacteria rids itself of Porine Ompts. At the same time, so-called lipopolysaccharides (LPS) are also repelled. These have insufficient resistance to the body’s defense mechanisms and are replaced by new LPS. These are tightly chained together and can strengthen the impermeability of the membrane.
The human body’s defense mechanism
This is activated by a defensive mechanism of the human body. Like the human body, the cholera bacterium requires the trace element iron for all biological processes. The body binds the iron in order to keep it from the intruder. Iron deficiency causes stress in the cholera bacteria, which react by repelling the OMVs (vesiculation). This gives the pathogens a clear advantage when colonizing the host.
Antibiotics can also help harmful bacteria
In addition, there are indications that contact with antibiotics or disinfectants in low doses can also lead to such occlusion. The molecular biologist concludes from this that residues of germicides in water or food can be a problem because they can give cholera bacteria a “fitness advantage.”
New therapeutic approaches
The phenomenon of the survival mechanisms of the cholera bacterium Vibrio cholerae apply to almost all bacterial pathogens including salmonella, pseudomonads or neisseria.
The findings are now being used for new therapeutic approaches to infectious diseases. Researchers are looking for a substance that inhibits the formation of these bulges. This would make it easier for the body’s own immune system to deal with the invaders. These new drugs could replace antibiotics and thus save the natural microbiome in the intestine.
Publications:
Franz G. Zingl, Paul Kohl, Fatih Cakar, Deborah R. Leitner, Fabian Mitterer, Katherine E. Bonnington, Gerald N. Rechberger, Meta J. Kuehn, Ziqiang Guan, Joachim Reidl, Stefan Schild, “Outer Membrane Vesiculation Facilitates Surface Exchange and In Vivo Adaptation of Vibrio cholerae”, Cell Host & Microbe, DOI: 10.1016/y.chom.2019.12.002
Also of interest: How we can reduce the risk of antibiotic resistance