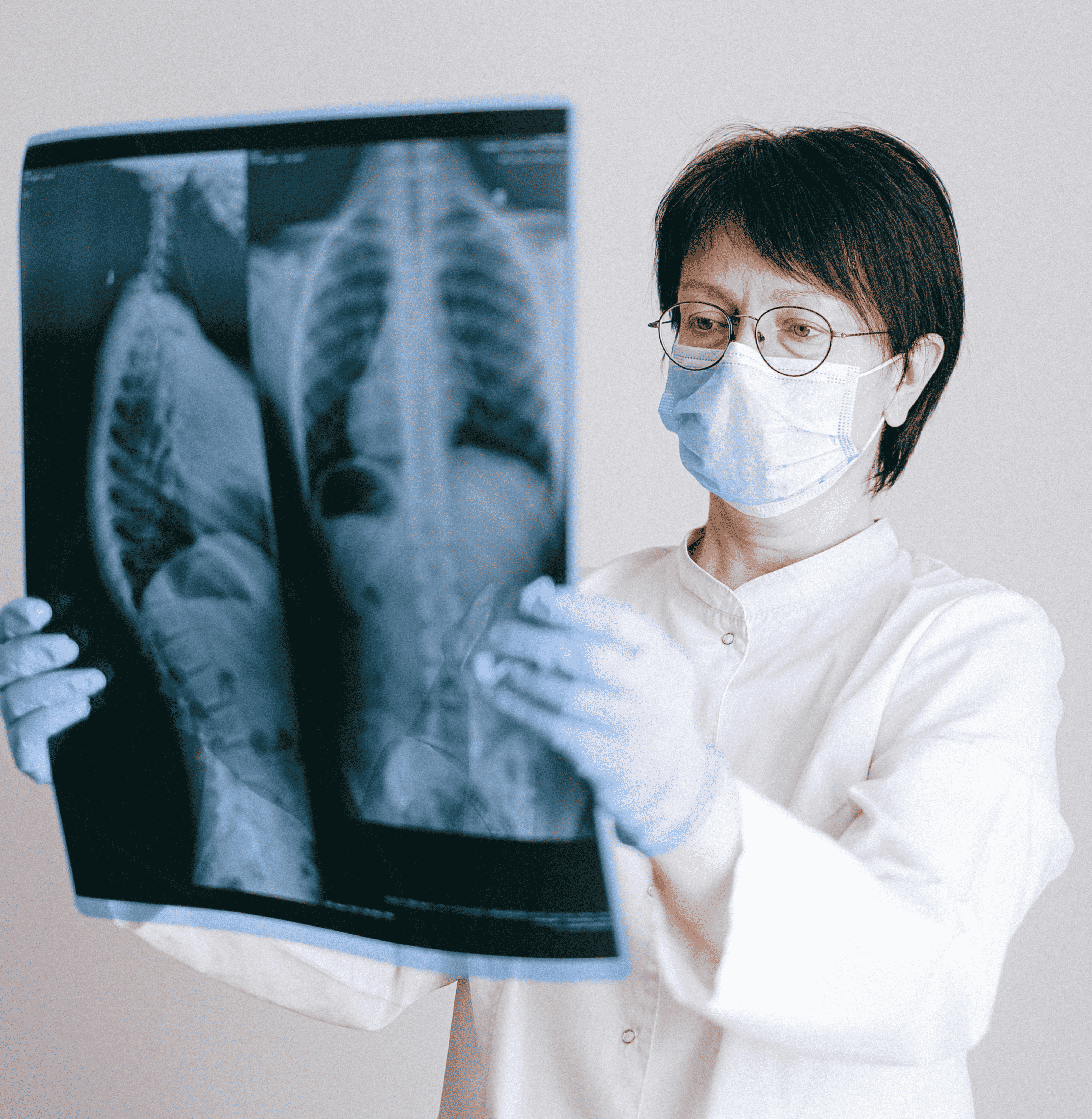
Corona patients with severe oxygen deficiency react positively to treatment with icatibant. A study by Radboudumc now results in follow-up research in ten Dutch hospitals into the effect of a drug that may be even more effective.
We wrote before about the start of this study
The rapid ‘filling’ of the lungs (pulmonary edema) is a characteristic of a serious infection with SARS-CoV-2 or Corona. Earlier, the Nijmegen researchers suggested that this has to do with the ACE2 (angiotensin-covering enzyme 2) receptor. The coronavirus penetrates the cells through this receptor, after which the virus can multiply.
However, the ACE2 receptor is not only the gateway for the coronavirus, it also controls vasodilating quinines. As a result of the infection, the ACE2 receptors disappear from the lung cells. Without ACE2 these quinines have free play and – by binding to bradykinin receptors – can make the blood vessels leak. Internist Frank van de Veerdonk, hospital pharmacist Roger Brüggemann and colleagues had the idea that this process plays an important role in serious coronavirus infection.
Patient survey
To determine whether a hypothesis is correct, you need to test. After consultation with the Committee on Human Subjects Research (CMO) and the Inspectorate for Health Care and Youth (IGJ) and with the consent of the participating patients, this was done with the medicine icatibant. Van de Veerdonk: “This medicine is used in patients with the rare condition hereditary angioedema. These patients sometimes suddenly develop severe subcutaneous fluid accumulation because their blood vessels start leaking locally. Icatibant blocks the bradykinin receptor B2R so that the leakage is quickly eliminated. To assess whether the drug is also suitable for the specific group of corona patients with fluid in the lungs, we administered it in the first half of this year to nine patients in the Internal Medicine department and one patient in the Intensive Care department.”
Immediate results visible
The results are now published in JAMA Network Open. All patients with severe oxygen deficiency due to fluid in the lungs were given subcutaneous injections of icatibant three times every six hours. The patient in the ICU could go to the ward 24 hours later and was discharged after 7 days. Eight of the remaining nine patients could do with a reduced amount of oxygen within 24 hours and the ninth after 38 hours. In eighteen comparable patients who acted as control groups, the decrease in oxygen delivery was significantly less.
Brüggemann: “In an early phase of the infection with severe oxygen deficiency, we see that icatibant improves the situation. One drawback is the short duration of the drug’s action. In two hours, half of the medicine has broken down, causing the effect to diminish rapidly. After treatment, three patients had to be given oxygen again because the drug had worn off.”
Other medicine
The researchers expect even better effects from another drug. Brüggemann: “The lanadelumab drug remains active much longer compared to icatibant, so you probably only need to administer it once or twice.” Van de Veerdonk: “Moreover, it has a much wider effect. It inhibits the activation of the entire system that causes the leakage of blood vessels. In short: it works longer and more comprehensively.”
International
Based on the initial results and these new insights, Van de Veerdonk and Brüggemann received a grant from ZonMw for a phase 2 clinical trial with lanadelumab for this specific group of COVID-19 patients. Ten hospitals are participating in the study. Brüggemann and Van de Veerdonk intend to roll out the study on an international scale. This is, they say, not only important for patients with severe oxygen deficiency but can also reduce the pressure on the IC capacity.